Wound Healing
What Is Wound Healing?
Wound healing is the body’s natural and highly coordinated biological process that repairs damaged tissue following injury, surgery, burns, trauma, ulcers, or chronic skin breakdown. This process involves a series of complex cellular and biochemical events designed to stop bleeding, prevent infection, rebuild tissue, and remodel the affected area until recovery is complete.
Under normal conditions, minor wounds heal efficiently through structured phases—hemostasis, inflammation, proliferation, and remodeling. However, certain medical conditions, impaired circulation, metabolic disorders, infection, or immune dysfunction can interrupt this healing cascade. When the process stalls, wounds may become delayed or chronic.
Chronic wounds, including diabetic foot ulcers, venous ulcers, and pressure injuries, represent a significant healthcare challenge and can severely affect mobility, independence, and overall quality of life. Understanding the mechanisms behind wound healing allows for earlier intervention, improved recovery, and reduced risk of complications.
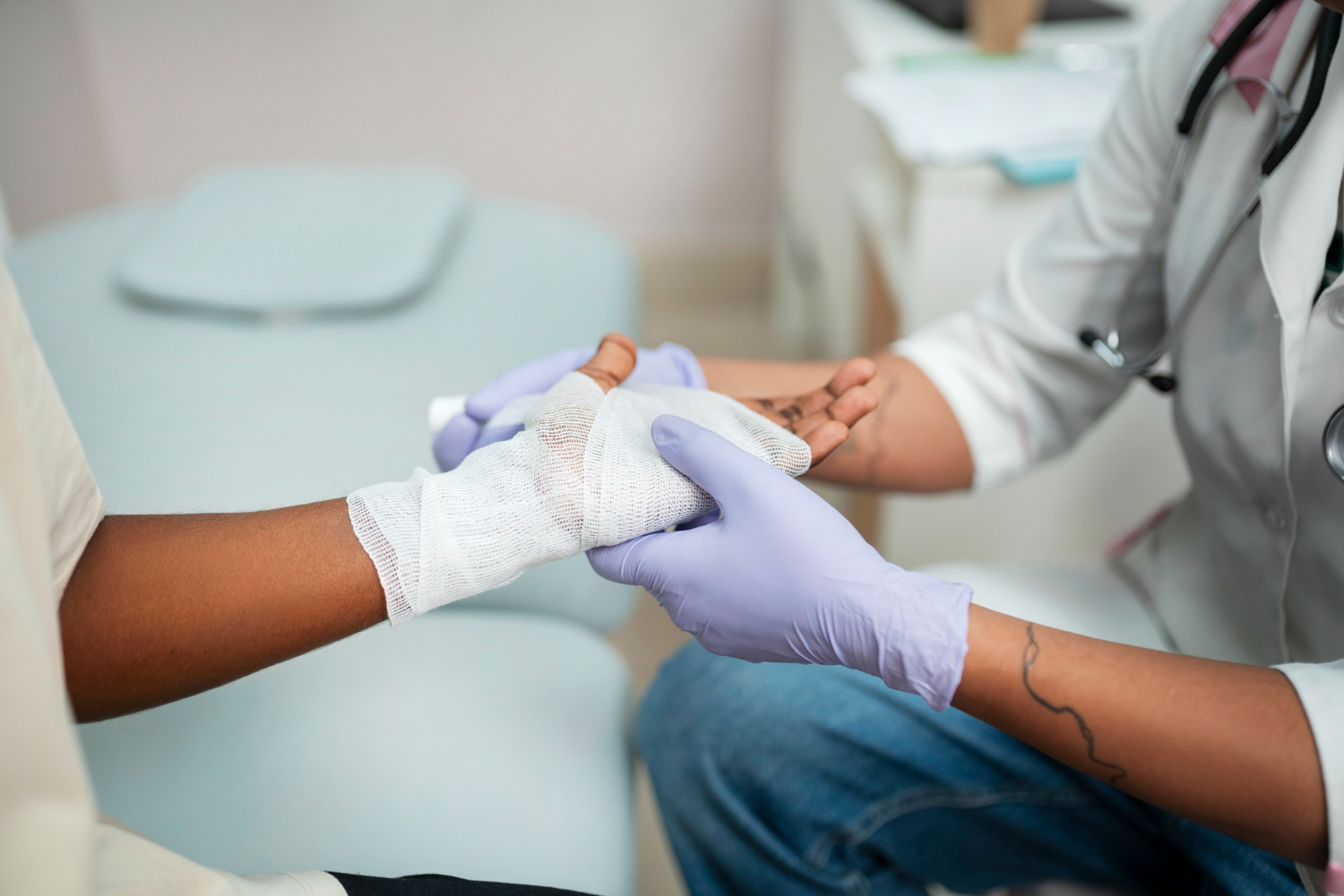
Causes of Delayed or Impaired Wound Healing
Wounds fail to heal properly for various reasons, most commonly related to poor circulation or underlying systemic disease. Conditions such as diabetes, peripheral artery disease, and venous insufficiency reduce oxygen and nutrient delivery to tissues, slowing regeneration. Diabetes, in particular, damages nerves and weakens immune response, increasing infection risk.
Prolonged pressure on specific areas of the body, especially in individuals with limited mobility, can cause pressure injuries that progressively damage skin and soft tissue. Repetitive friction, poorly fitting footwear, or trauma may also initiate chronic wound formation.
Immune dysfunction, advanced age, obesity, autoimmune disease, and chronic inflammation further impair tissue repair. Infection plays a major role in delayed healing, as bacteria disrupt normal cellular activity and prolong inflammation. Nutritional deficiencies, dehydration, smoking, and certain medications also interfere with the body’s regenerative capacity.
Addressing these contributing factors is essential for restoring effective healing.
Symptoms of Impaired Wound Healing
Signs of abnormal healing vary depending on the wound’s severity and duration. Early symptoms often include persistent redness, swelling, warmth, tenderness, or pain around the affected area. The wound may fail to shrink over time or may deepen instead of closing.
Other warning signs include excessive drainage, foul odor, tissue discoloration, or necrosis. Infected wounds may cause fever, chills, fatigue, or increasing discomfort. Changes in skin texture, surrounding discoloration, or spreading redness may signal worsening inflammation.
Recognizing these symptoms early and seeking medical evaluation can significantly reduce the risk of serious complications.
How Many People Are Affected?
Chronic wounds affect more than 6.5 million people annually, with prevalence continuing to rise due to aging populations and increasing rates of diabetes and vascular disease. Older adults, individuals with limited mobility, and those with chronic illnesses are particularly vulnerable.
Because non-healing wounds impact independence, mobility, and emotional well-being, early awareness and proactive treatment are essential for improving long-term outcomes.
Potential Complications
Untreated or poorly managed wounds can lead to serious complications. Infection is among the most immediate risks and may spread to surrounding tissue, resulting in cellulitis, abscess formation, osteomyelitis, or systemic sepsis. Persistent inflammation can destroy healthy tissue, causing wounds to enlarge or deepen.
In severe cases, particularly among individuals with poor circulation, necrosis or gangrene may develop. Recurrent wounds are common in patients with diabetes or vascular insufficiency. Beyond physical risks, chronic wounds may contribute to anxiety, depression, and reduced quality of life.
Amputation remains one of the most severe complications of non-healing diabetic foot ulcers. Early diagnosis and structured management significantly reduce this risk.
Diagnosis
Diagnosis begins with a comprehensive clinical evaluation of the wound’s size, depth, duration, and surrounding tissue condition. Medical history, circulation status, blood sugar control, and underlying health conditions are assessed to determine contributing factors.
Diagnostic testing may include blood work to evaluate infection markers, glucose levels, and nutritional status. Vascular studies may assess arterial or venous circulation. In certain cases, imaging may be performed to evaluate deeper tissue involvement or bone infection.
Accurate diagnosis allows clinicians to develop a targeted and individualized treatment plan that addresses both the wound and its underlying cause.
Treatment Options
Wound healing treatment focuses on correcting underlying conditions, promoting tissue regeneration, preventing infection, and restoring skin integrity. Proper wound cleansing and sterile protection are foundational components of care. Debridement may be necessary to remove necrotic or infected tissue and create a healthy environment for healing.
Maintaining a balanced moisture environment is essential. Advanced dressings, gels, foams, and barrier films help regulate hydration and protect against contamination. When infection is present, antibiotics may be prescribed based on clinical evaluation.
Offloading pressure—particularly for diabetic foot ulcers—is critical. This may involve orthotics, specialized footwear, casting, or pressure redistribution devices. Optimizing blood sugar control significantly improves healing outcomes for individuals with diabetes.
Improving circulation through medical management, lifestyle modification, or procedural intervention may also be required. Nutritional optimization, smoking cessation, hydration, and physical therapy further support tissue repair.
For appropriate candidates, advanced regenerative therapies such as platelet-rich plasma (PRP), exosomes, stem cell applications, low-level light therapy (LLLT), peptides, diagnostic ultrasound, microneedling, or shockwave therapy may be considered to enhance tissue recovery and cellular repair.
Ongoing follow-up ensures healing progression and early detection of complications.
Resources
SCHEDULE A CONSULTATION
Schedule Your Orthopedic Consultation
If you are experiencing persistent shoulder or knee concerns and would like to explore whether regenerative therapies may be appropriate, we invite you to schedule a consultation.
